Findings from a Systematic Literature Review
Evidence suggests that simply increasing knowledge and awareness of good nutrition practices rarely leads to sustained behavior change. In addition, sustained change in nutrition behavior is unlikely to be achieved through a single activity. Several specific behaviors or practices impact nutritional status during the critical first 1,000 days (pregnancy to age two), while complex contextual determinants also influence individual decisions to consider, test, adopt, and sustain a given behavior or practice. The field of social and behavior change communication (SBCC) is a collection of approaches and tools informed by behavioral theories and used to design public health interventions.
In an effort to support governments and other stakeholders in their delivery of high-impact nutrition practices, SPRING conducted a systematic review of peer-reviewed evidence regarding the effectiveness of SBCC approaches to increase the uptake of three key nutrition behaviors:
- women's dietary practices during pregnancy and lactation
- breastfeeding practices
- complementary feeding practices.
This review also identifies gaps in the evidence and provides recommendations for further areas of study. The SBCC interventions included in the review can be broadly categorized into three areas: interpersonal communication, use of media, and community/social mobilization. The review includes 91 studies, and results from reviews (including meta-analysis), randomized controlled trials, longitudinal studies, repeated cross-sectional studies, and cross-sectional studies. For a full description of methods used, please see the full report (PDF, 1 MB).
Findings
Table 1: Number of Studies by Intervention Area and Study Design
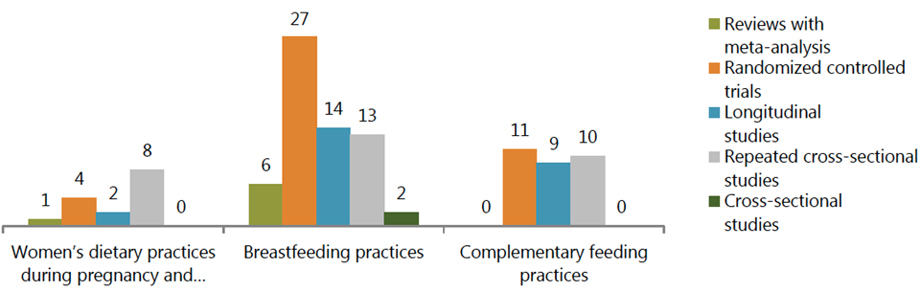
Women's dietary practices during pregnancy and lactation
Undernutrition during pregnancy and lactation is a critical determinant of maternal, neonatal, and child health outcomes. Improving dietary adequacy during this period is important to help women fulfill their nutritional requirements and their children's requirements during intrauterine development and while breastfeeding.1
The body of literature on the effectiveness of SBCC to improve women's dietary practices during pregnancy and lactation is still small (only 15 peer-reviewed studies met the inclusion criteria), but indicates that SBCC approaches can and do succeed in improving uptake of the behaviors promoted. The greatest gap in the literature was in evidence of the effectiveness of SBCC in improving rest and workload during pregnancy. Given the importance of women's dietary practices during pregnancy and lactation, the dearth of evidence is notable.
Browse this section's interactive table of articles

Findings related to breastfeeding practices
Breastfeeding is widely recognized as one of the most cost-effective investments for improving child survival,2 as well as cognitive and motor development, and academic performance.3 Breastfeeding also imparts critical benefits to women, including natural postnatal infertility. Despite the promise of optimal breastfeeding practices, rates for WHO-recommended breastfeeding practices remain low.2
The body of literature on the effectiveness of SBCC approaches in improving breastfeeding practices is strong and broad (62 peer-reviewed studies met the inclusion criteria) and supports the claim that SBCC approaches can and do succeed in improving uptake of the behaviors promoted.
Evidence from several studies strongly suggests that increasing the number of contacts increases the positive effect of SBCC on breastfeeding practices. How breastfeeding practices are measured – the definitions of indicators and the methods of data collection – is more consistent than how women's dietary practices and complementary feeding practices are measured, but even with globally-recognized indicators and measurement guidance, considerable variation remains.
Browse this section's interactive table of articles
Findings related to complementary feeding practices
Timely, appropriate complementary feeding is critical to a child's growth and development and could avert millions of disability-adjusted life years,4 but global coverage of optimal complementary feeding practices remains low.5
Evidence of the effect of SBCC on complementary feeding practices is quite broad (30 peer-reviewed studies met the inclusion criteria) and clearly indicates that SBCC interventions can improve a wide range of complementary feeding practices. However, measures of optimal complementary feeding are so varied that it is particularly challenging to draw conclusions regarding the effectiveness of particular approaches.
Browse this section's interactive table of articles
Common findings
Interpersonal communication (IPC) is most commonly used: IPC was the SBCC approach most used, and the only one used without other communication interventions. While media and community/ social mobilization were used, they were always used with at least one other communication approach.
There is a wide range of implementation strategies: The range of implementation strategies included variations in the interactions or combinations with other interventions, target groups, content, messages, scale and coverage, length and intensity, as well as context.
Very little has been done to compare the effect of differences in delivery: This is particularly apparent for interventions implemented at scale.
The majority of the studies were implemented on a small scale: Typically, studies included fewer than 500 people per group.
There is significant variation in definitions and measurement: This is especially varied for women's dietary practices and complementary feeding practices.
Conclusions

Evidence suggests that using multiple SBCC approaches and channels to change behaviors is more effective than using one, that targeting multiple contacts has a greater effect than targeting only the woman herself, and that more visits or contacts results in greater change. However, such comparisons are not well-tested in the literature. Additionally, little has been done to determine when during a woman's pregnancy or a child's life practices should be promoted; what little has been done presents contradictory evidence. Unfortunately, it can be challenging to conduct studies that compare differences in delivery and to disaggregate single approaches within a multi-approach intervention. SBCC practitioners and researchers must assess whether that line of research is useful.
Differences in local context (including social norms, culture, and environmental factors), implementation methods, and implementation scale also affect intervention success. This underscores the importance of proper context assessments, formative research and/or ethnographic study prior to SBCC implementation.
Finally, if practices and indicators are not standardized, a project may improve behaviors, but it will be difficult to attribute changes in outcomes. This underscores the importance of developing practices and indicators that are globally recognized, accepted, and used by the research and program communities. At the same time, many nutrition interventions are suited to iterative programming for incremental change toward optimal, evidence-based behaviors. This means that more easily achieved indicators (components of standardized indicators or shorter time periods) may also be needed to measure progress toward the ultimate goal of changes in the standardized indicators of behaviors.
Recommendations
In addition to creating standardized definitions and indicators for these practices, other areas particularly important for future evaluations and operations research include—
- the effect of targeting multiple audiences or influencers of the behaviors being promoted, rather than focusing on one target population
- the effect of the same SBCC intervention implemented in different contexts (social and environmental)
- the effectiveness of different approaches (including intensity and targeting) for different behaviors
- the cost and cost effectiveness of various SBCC approaches (particularly as they relate to scalability)
- the effectiveness and sustainability of these approaches when implemented at scale.
Footnotes
1 Haileslassie K, Mulugeta A, and Girma M. 2013. “Feeding Practices, Nutritional Status and Associated Factors of Lactating Women in Samre Woreda, South Eastern Zone of Tigray, Ethiopia.” Nutrition Journal 12 (1): 28
2 UNICEF. Improving Child Nutrition: The achievable imperative for global progress. New York: UNICEF, 2013.
3 Horta, B, Bahl R, Martines J, Victora C. Evidence on the long-term effects of breastfeeding. Geneva: World Health Organization, 2007.
4 Bhutta ZA, Ahmed T, Black RE, Cousens S, Dewey K, Giugliani E, Haider BA, et al. 2008a. “What Works? Interventions for Maternal and Child Undernutrition and Survival.” The Lancet 371 (9610) (February): 417–440
5 Lutter, CK, Daelmans BM, de Onis M, Kothari M, Ruel MT, Arimond M, Deitchler M, Dewey KG, Blossner M, Borghi E. (2007). “Undernutrition, poor feeding practices, and low coverage of key nutrition interventions.” Pediatrics. 128(6), e1418-1427.



